Protection Against Aspiration And Gastric Insufflation
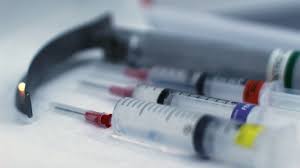
Upon waking, a person who has been intubated can experience a sore throat, difficulty swallowing or discomfort within swollen regions of the face or neck. Salivary pooling (see bubbles) is seen, likely due to interference with swallowing caused by topical anesthesia. It can however be performed in an emergency without any anesthesia at all. Because intubation is an invasive and extremely uncomfortable medical procedure, it is usually performed after administration of general anesthesia and a neuromuscular-blocking drug(muscle relaxants or paralysing agents). In this study, researchers hoped to identify whether there was a statistically significant difference in neurologic outcome in patients who had a supraglottic airway insertion versus tracheal intubation. The researchers concluded that use of a supraglottic airway device did not result in favorable neurologic outcomes at 30 days when compared with tracheal intubation. A total of 764 paramedics were randomly assigned to perform tracheal intubation, and 759 paramedics were randomly assigned to perform supraglottic airway device placement. Overall, 4886 patients received the supraglottic airway device and 4410 patients underwent tracheal intubation. Although the numbers of paramedics randomly assigned to each trial arm were roughly the same, paramedics in the supraglottic airway group were more likely to perform this advanced airway management technique than paramedics in the tracheal intubation group.
Researchers also found that the incidence of aspiration and regurgitation was more likely after supraglottic airway placement but before tracheal intubation. At closer range, divots begin to be appreciated (above the X’s) and bilateral glottic furrows are more clearly noted. This type is performed much more frequently than nasotracheal intubation. The researchers made interesting observations about the decision-making process for the type of airway to use. Intubation has a number of risks, such as inadvertently placing the endotracheal tube in the stomach instead of the esophagus or puncturing the esophagus in the process of insertion. Listening over apices and bases of lungs and stomach for equal breath sounds and no gastric breath sounds. If the tube is placed in the esophagus instead of the trachea, oxygen can enter the stomach and cause cardiac arrest, ARDS, brain damage, and even death. The tube validates the sufficient exchange of oxygen and carbon dioxide along with preserving the patient’s airway. Intended for assisted fiberoptic intubation and for uncomplicated, atraumatic endotracheal tube exchange.
A patient with respiratory failure may require endotracheal intubation (31500 Intubation, endotracheal, emergency procedure) for airway support. Normally, it is difficult for a Patient to tolerate a breathing tube and your loved is very likely getting sedative drugs(Propofol or Midazolam) and pain medication(Morphine or Fentanyl), in order to be able to let the ventilator do its work. In order to post comments, please make sure JavaScript and Cookies are enabled, and reload the page. There is air wasting through the posterior keyhole not visible here, and the bilateral glottic furrows and pseudo-bowing are extremely evident. There were doctors rushing around “just like an ER here,” Greenough said. Here, the right vocal cord (left of photo) appears atrophied (spaghetti-lunguini larynx). Under strobe light, during the closed phase of vibration, vocal cord closure appears to be firm and equal bilaterally. At closer range, intubacao aperfeicoamento orotraqueal, the right vocal cord (left of photo) appears normal; the left (right of photo) appears to have much less bulk.
At close range, the area of posterior scarring is again indicated by dotted line; the dark area of the actual airway is narrow and slit-like. Tip of the iceberg view of granulation and scarred area. White-out of the large area of the upper surface is mostly from over-illumination. While the right cord appeared atrophied, it shows no flaccidity. However, the new research shows that while hyperventilation lowers that pressure, it also deprives the brain of blood and oxygen. By using her EPIC training, Alex Matthews focused on preventing what the researchers call the “Three H-bombs” — hyperventilation, hypoxia and hypotension, or, in everyday language, rapid breathing, oxygen deprivation and low blood pressure. In this view with vocal cords abducted for breathing, the left vocal cord (right of photo) manifests an increase in vascularity and a margin swelling posteriorly (at arrow). The vascular pattern of the right cord (left of photo) is normal.
Focus on the damaged left vocal cord (right of photo) for the rest of this series. During the days following a severe flare, it is appropriate to rest and avoid physical activity although this should be just for a brief period. Airway is no longer marginal, but is still very limited for significant activity. Some of the dreams were linked together as parts of a longer narrative. Airway Grade is what you see in the posterior pharynx with a laryngoscope. A month after posterior commissuroplasty, breathing is improved due to the widened space posteriorly. Placement of her breathing tube was said to be difficult. Generally, there will be documentation stating CO2 indicator or X-ray confirmation of placement. Your vet will use tongs padded with a sponge to grasp your dog’s tongue and move it gently to the side to allow for proper tube placement. Oxygen, anesthesia, or a mix of gasses will then be administered by connecting the tube to the appropriate machine.







